Imagine you're at a doctor's office or home, and shortly after taking a new prescription, your throat begins to tighten and your heart starts racing. This isn't a mild itch or a few hives; it's a medical emergency. Anaphylaxis is a severe, life-threatening systemic allergic reaction that causes rapid failure of the airway, breathing, and circulation (ABC). When triggered by medication, it can happen in seconds, leaving almost no room for hesitation. If you or someone else experiences this, knowing the exact sequence of steps to take can be the difference between a quick recovery and a fatal outcome.
Spotting the Signs Fast
The biggest hurdle in saving a life during a drug reaction is often hesitation. Many people wait for a rash to appear, but the 2022 Journal of Emergency Medicine notes that skin changes are actually absent in 10-20% of cases. You cannot rely on hives alone to diagnose the situation.
Watch for these red flags, which often appear suddenly:
- Breathing issues: Noisy breathing, wheezing, a persistent cough, or a hoarse voice.
- Swelling: A swollen tongue or a feeling of tightness in the throat.
- Circulation failure: Sudden dizziness, feeling faint, or a complete collapse.
- Pediatric signs: In young children, look for a sudden, ghostly pale appearance.
If you see a combination of these symptoms following the administration of a drug-especially antibiotics like penicillins, NSAIDs, or chemotherapy agents-you must act immediately. In the world of emergency medicine, the rule is simple: if you're in doubt, give the adrenaline.
The Critical First Move: Proper Positioning
Before you even reach for the medicine, you have to get the person in the right position. This is where most people make a mistake. Your instinct might be to help someone sit up to breathe better or let them walk to a chair, but doing so can be deadly. According to the Resuscitation Council UK, changing position from lying flat to standing is linked to cardiovascular collapse in 15-20% of cases.
Follow these positioning rules strictly:
- Standard response: Lay the person flat on their back immediately.
- Breathing difficulty: If they are struggling to breathe, they can sit up, but keep their legs outstretched.
- Unconscious or Pregnant: Use the recovery position. For pregnant women, ensure they are lying on their left side to keep blood flowing to the heart.
- Children: Keep young children flat on their backs; do not hold them upright.

Step-by-Step Emergency Medication
The only treatment that can reverse the systemic collapse of anaphylaxis is Epinephrine (also known as Adrenaline). Antihistamines like Benadryl might stop a few itchy spots, but they do absolutely nothing to open a closing airway or raise plummeting blood pressure. Every second counts; the goal is to administer the dose within 5 minutes of the first symptom.
| Patient Weight | Recommended Dose | Administration Site |
|---|---|---|
| Adults & Children > 30 kg | 0.3 mg | Outer thigh (Anterolateral) |
| Children 15-30 kg | 0.15 mg | Outer thigh (Anterolateral) |
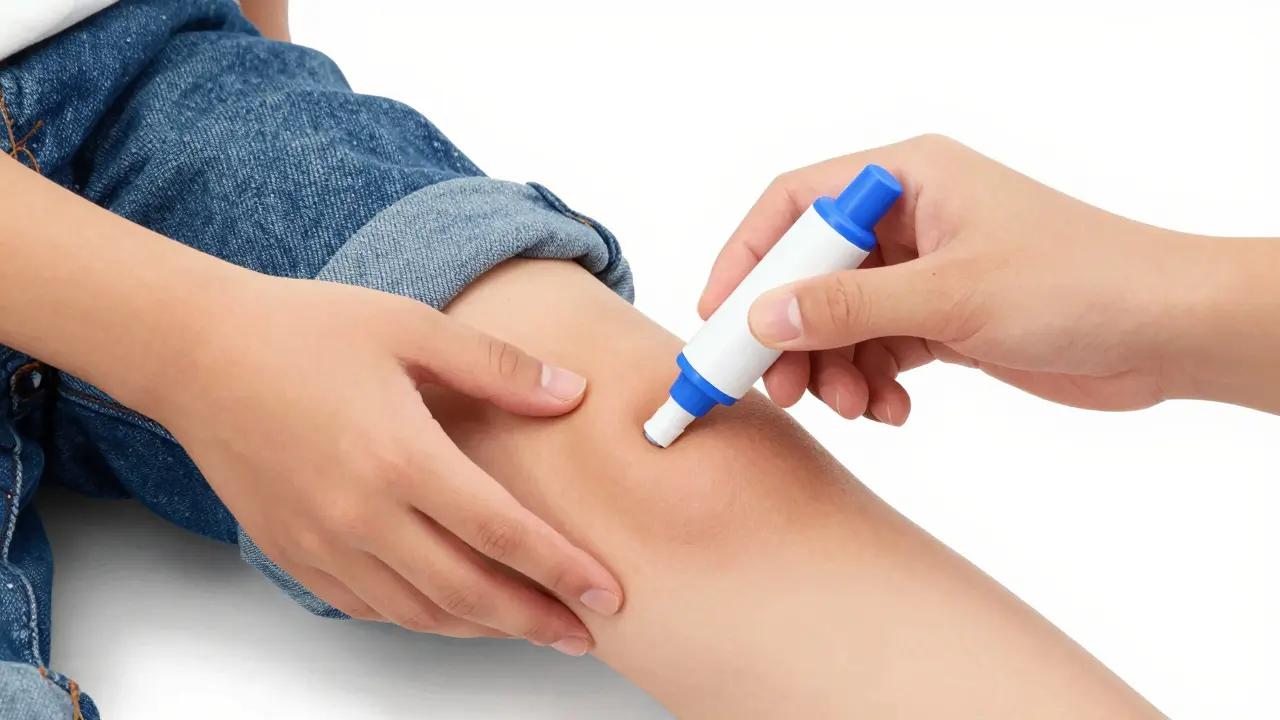
To use an Epinephrine Auto-Injector (such as an EpiPen, Auvi-Q, or Adrenaclick), follow these precise steps:
- Prepare: Remove the safety cap.
- Inject: Press the device firmly into the outer mid-thigh. You can do this right through clothing if necessary.
- Hold: Keep the device pressed against the thigh for a full 10 seconds. Many people pull it away too early, leading to an incomplete dose.
- Massage: Gently rub the area for a few seconds to help the medication absorb.
Remember that epinephrine is short-acting. It typically works within a few minutes but wears off in 10 to 20 minutes. If the breathing problems or dizziness don't improve or they start to return after 5 minutes, administer a second dose in the opposite thigh.
What Happens Next: The Hospital Phase
Even if the person seems completely fine after the injection, you cannot go home. You must call emergency services immediately. There is a dangerous phenomenon known as a biphasic reaction, where the symptoms return hours after the first attack. This happens in about 20% of cases, and for medication-induced reactions, the risk is even higher-potentially 25%-compared to food allergies.
Medical professionals will typically keep a patient under observation for 4 to 8 hours. In a hospital setting, doctors may use IV Fluid Resuscitation, pumping 1-2 liters of normal saline into the bloodstream to stabilize blood pressure. This is especially critical for patients in shock, as it significantly reduces the risk of death when paired with epinephrine.
Common Pitfalls and Expert Warnings
There are a few "old school" medical habits that are now considered dangerous or ineffective. For instance, many people reach for corticosteroids (like hydrocortisone). Modern guidelines from the Cleveland Clinic state that these are no longer recommended for routine treatment because they take too long to work and don't stop the immediate life-threatening collapse.
Another critical factor is the use of beta-blockers. If a person takes medication for high blood pressure (specifically beta-blockers), standard doses of epinephrine might not work. In these cases, they may need 2-3 times the usual dose to get a therapeutic response. This is why telling the emergency team exactly what medications the patient takes is vital.
Can I use an antihistamine instead of an EpiPen?
No. Antihistamines only treat skin-level symptoms like itching or hives. They cannot stop the throat from closing or prevent a drop in blood pressure. Epinephrine is the only first-line treatment for anaphylaxis.
What if I'm not sure if it's anaphylaxis or just a mild reaction?
If you see signs of airway, breathing, or circulation problems (like swelling or dizziness), administer the epinephrine immediately. The risk of not treating anaphylaxis is far higher than the risk of giving an unnecessary dose of adrenaline.
Why should the patient stay lying down?
Standing up during a reaction can cause a sudden drop in blood pressure, leading to cardiovascular collapse and death. Keeping the patient flat helps maintain blood flow to the heart and brain.
How long does the effect of the auto-injector last?
The effects typically last 10 to 20 minutes. This is why professional medical monitoring is required and why a second dose may be necessary if symptoms persist beyond 5 minutes.
Which medications are the most common triggers?
Antibiotics (especially penicillins) are the most common, accounting for nearly half of medication-induced fatalities. NSAIDs and neuromuscular blocking agents used in anesthesia are also frequent triggers.




9 Comments
This is a great reminder about the positioning. A lot of people instinctively try to sit someone up to help them breathe but that actually messes with the blood pressure and makes things way worse.
Absolutely spot on regarding the biphasic reaction. It is so critical to avoid the temptation of early discharge because that secondary surge of inflammatory mediators can be just as lethal as the initial trigger. Always maintain clinical observation :)
they dont tell you about the other stuff they put in the pens to make you dependent on the system
USA healthcare is still the best even with the cost 🇺🇸🇺🇸 just glad we got these tools to save lives lol its crazy how some ppl dont know about the legs thing!! 😱
honestly it is just typical that people have to be told to lie flat because common sense has completely disappeared in this generation and i find it slightly exhausting that we need a whole guide for something that should be intuitive if you actually paid attention to basic biology but whatever i guess
Cut the attitude. This info saves lives regardless of whether you think it is common sense or not 🙄👊
imagine thinking the US has the best care when my countrys doctors are far more rigorous in their training and we handle these emergencies with way more grace and precision than the clumsy western approach 🇮🇳🇮🇳 superiority is real
For anyone feeling overwhelmed by this, just remember that practicing the steps of using a trainer pen (the ones without needles) can build the muscle memory you need to stay calm in a real crisis. You've got this!
Stay safe everyone 🌸✨